I have written previously on the role of the epiglottis in obstructive sleep apnea. My colleagues around the world largely agree that the epiglottis plays an important role in about 10% of patients with obstructive sleep apnea. However, there is much that we do not know, including why epiglottis-related obstruction occurs in some patients but not others.
My own experience is that epiglottis-related obstruction is more common in older adults with sleep apnea, especially in those who have significant obstructive sleep apnea in spite of being relatively thin (making one think they should not have sleep apnea at all). Based on this observation, I worked with one of our former residents in the USC Caruso Department of Otolaryngolgy–Head & Neck Surgery, Leslie Irvine, MD, to perform some research that examined the potential role of aging in epiglottis-related obstruction.
Obstructive sleep apnea and aging
Obstructive sleep apnea is more common with increases in age, reaching a plateau after age 60. There are probably many factors that can explain this, but these same soft tissue changes likely play a role. It appears that the epiglottis can play a role in obstructive sleep apnea by being too large, too floppy, or too mobile, meaning that it is not held firmly in a position to keep the airway open.
It is no secret that aging is associated with changes in our skin and other soft tissues. In short, people develop skin wrinkles and sagging in other areas as we get older because of increased looseness, or laxity, of our our soft tissues. This occurs because of changes in collagen, elastin, and other fibers within the soft tissues that provide strength and resilience. However, aging does not affect all soft tissues equally.
Dr. Irvine’s Research Here at USC
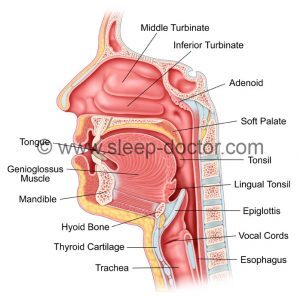
The hyoepiglottic ligament connects the epiglottis with the hyoid bone and is one of the key anchors for the epiglottis. Laxity of the hyoepiglottic ligament could contribute to epiglottis-related obstruction by allowing the epiglottis to fall backwards and block breathing during sleep. Dr. Irvine examined 25 cadaver hyoepiglottic ligamentsa cross a wide age range and worked with the team of Bo Han, PhD of the Department of Surgery at the Keck School of Medicine of USC. Her research showed that age was associated with a decrease in collagen and elastin fiber density within the hyoepiglottic ligament, using statistics to control for any history of smoking (another cause of collagen changes in soft tissues).
This has important implications for epiglottis-related obstruction in sleep apnea. First, it supports the above explanation as one factor in the increased risk of obstructive sleep apnea associated with aging. Second, it suggests that the hyoid suspension procedure may represent a reasonable treatment of epiglottis-related obstruction, as holding the hyoid bone in a forward position may address the hyoepiglottic ligament laxity more directly. The primary downside to hyoid suspension is the risk of difficulty swallowing, with one recent study suggesting that trouble swallowing may be more common after hyoid suspension than other sleep apnea procedures, at least in the first couple of months after surgery. The other approach for epiglottis-related obstruction is epiglottis surgery, and this may be be better in cases where the epiglottis is especially large or floppy.




joseph enrico carbone says:
How much of the epiglottis is recommended to do in a resection
Dr. Kezirian says:
There is no single answer, and experienced surgeons have different opinions. My approach is to perform the procedure differently in different patients, often using drug-induced sleep endoscopy to guide the decision.