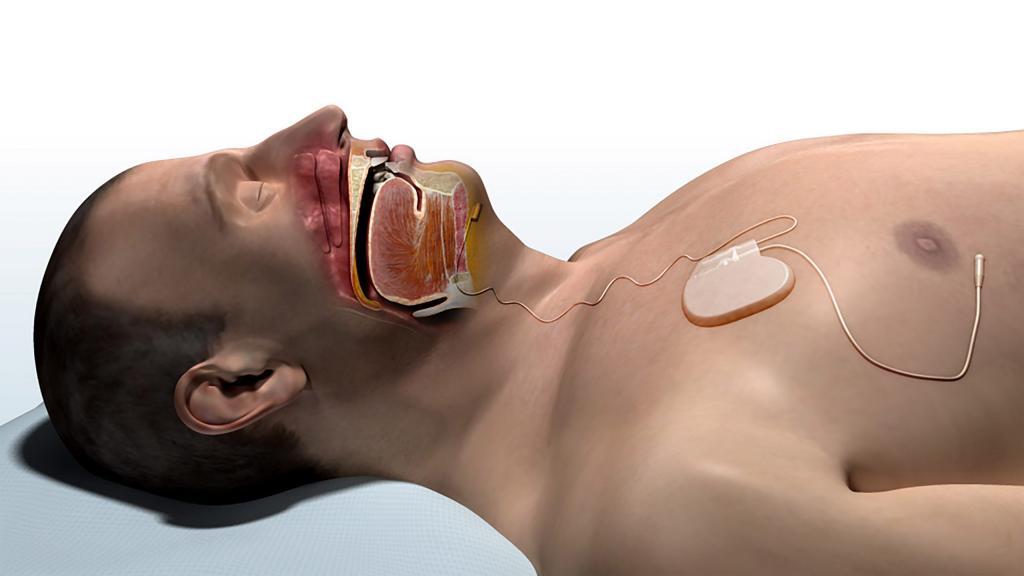
Inspire Medical Systems received FDA approval in 2014 for their Upper Airway Stimulation therapy to treat obstructive sleep apnea, and we were the first center in the Western United States to offer this treatment to patients after that approval. We have a substantial experience with this therapy here and have always felt it essential to discuss it as an important option that can provide excellent results for many patients with obstructive sleep apnea. This technology delivers electrical stimulation to the hypoglossal nerve, which is the nerve that controls tongue movement. This stimulation moves the tongue forward and can be exactly what a patient needs to open the space for breathing in their throat and treat their obstructive sleep apnea.
One of the most interesting things about the approval for Upper Airway Stimulation was the requirement that patients undergo drug-induced sleep endoscopy (DISE) before surgery as part of the eligibility process. DISE is an evaluation of patients under sedation designed to reproduce something close to natural sleep, and the purpose of DISE is to determine the physical causes of the blockage in breathing that occurs in obstructive sleep apnea. The requirement of DISE before implantation of the Upper Airway Stimulation system was based on a small study done early in the clinical testing that suggested that a DISE finding of what is called complete concentric collapse related to the soft palate (velum) was associated with poor outcomes. Based on this study, DISE was added as a requirement for enrollment in later studies of Upper Airway Stimulation, including the STAR Trial that showed substantial improvements in obstructive sleep apnea and served as the basis for FDA approval.
Can we use DISE findings in a better way?
DISE offers substantial information about the pattern of airway blockage overall, much more than just whether or not a patient had this one specific pattern of complete concentric collapse related to the soft palate. My feeling for a long time has been that we were not using DISE fully to guide the decision about whether Upper Airway Stimulation might achieve the results we want. To answer this question properly, you need large numbers of patients from multiple centers, and this is exactly the approach we took with our international, multicenter study showing an association between DISE findings and outcomes of other surgeries.
Last month, the medical journal Laryngoscope accepted for publication a similar study from our group. I am biased, but I really think this is an important contribution to improving the care of patients with obstructive sleep apnea. Philip Huyett, MD started this study when he was finishing his training with us at USC and finished the work as he joined the faculty at Massachusetts Eye and Ear. It was not a trivial effort. The centers (with coauthors) collected data from a total of 343 adults with obstructive sleep apnea who were treated with Upper Airway Stimulation across 10 centers. For each study participant, the center sent the actual video from their preoperative DISE evaluation. All videos were reviewed by four experienced sleep surgeons: Dr. Huyett; David Kent, MD from Vanderbilt; and Mark D’Agostino from the Southern New England Ear, Nose, Throat, & Facial Plastic Surgery Group and Yale; and me. We combined the scores into consensus scores of DISE findings and tested the association with outcomes of what is called the titration sleep study, in which a patient undergoes a sleep study in the sleep lab, with determination of optimal settings for the Upper Airway Stimulation system. The titration study is probably not the ideal setting to judge how well the system is working because the results on the optimal settings come from only part of the night (because many different settings are tested during the sleep study).
Important study results re: the tongue and sides of the throat
Overall, there were substantial improvements in obstructive sleep apnea with Upper Airway Stimulation, and 73% of the group achieved what would be considered a substantial improvement, at least according to the titration sleep study. For me, the two most important findings were related to DISE findings concerning the tongue and the side of the throat (oropharyngeal lateral walls). Importantly, the real impact is clearer when placed in context of our previous study of other sleep apnea procedures.
For the tongue, Upper Airway Stimulation results were better with complete blockage of breathing related to the tongue (78% response rate vs. 68% with either partial or no blockage related to the tongue; p-value = 0.043 for those who are interested). This almost seems counterintuitive, in that you might wonder why more blockage leads to better results. My best guess is that complete tongue-related obstruction suggests that the tongue is the key factor causing the obstructive sleep apnea, so a treatment that moves the tongue forward directly likely Upper Airway Stimulation would be expected to be perfectly suited to this therapy. This finding is even more important in light of our previous study that showed that complete tongue-related obstruction was associated with poorer outcomes from other procedures. The result is that I tell patients with complete tongue-related blockage that Upper Airway Stimulation may really be the right approach for them, as results are just better than other procedures, everything else being equal.
For the sides of the throat, the key finding seemed to be whether patients had complete blockage (vs. partial or none), as this was associated with poorer outcomes (58% vs. 74% response rates; p = 0.042). Importantly, partial blockage was not associated with poorer outcomes. One previous study has shown that one of the ways that hypoglossal nerve stimulation opened the space for breathing could be displacing the sides of the throat outwards (more open). We showed that this displacement might explain why patients with partial blockage related to the sides of the throat may still respond well, but this therapy may not be enough to achieve good results in patients with complete blocakge. Again, the full importance is seen by comparing it to our previous study results, where both partial and complete airway obstruction related to the sides of the throat was associated with poorer outcomes. For patients with blockage of breathing related to the sides of their throat – especially if that blockage is only partial – I do discuss this DISE finding as one to suggest that Upper Airway Stimulation might be particularly helpful.
I hope that this discussion has not been too technical. I write about this research because I feel that high-quality, scientific research can directly improve results for patients. I love performing research and using research to enhance the quality of discussions with my patients so that we can make informed decisions together.




Humberto Bringas says:
Hello Dr. Kezirian, I recently had the Inspire implant surgery on 9/29/21. It was actually activated on 11/13/21 so I have been using it for a little over a week now. I started on setting # 2 and I am now on setting 5. I am tolerating it fine. I don’t feel any difference other than my wife says I stopped snoring. I had a DISE procedure done in 2016 that my doctor was able to use to get my surgery approved through insurance, My sleep study was just done in July of 2021, and I was found to have severe obstructive sleep apnea with an AHI of 58.2 (central 11, obstructive 14, mixed 3, hypopnea 248). My question is based on the DISE findings below was I a good candidate for this surgery:
Velopharyngeal partial anterior-posterior collapse. Oropharyngeal , no collapse. Base of tongue, complete anterior-posterior collapse. Presence of lingual tonsils. Epiglottis, complete anterior-posterior collapse.
I feel you are very knowledgeable and would appreciate your input.
Thank you,
Bert
Question is, will the Inspire implant help me?
Dr. Kezirian says:
You should definitely remain in contact with your physicians. It is common not to experience benefit right away, although it sounds like your snoring is at least improving. You will almost certainly have an in-laboratory sleep study in 1-2 months, where the team will test how your sleep apnea is improving and what settings are ideal for you. The one concern I have is that you had a reasonable amount of central sleep apnea that can interfere with the proper working of the Inspire system, but the team will check that during the in-laboratory sleep study. This post is about the specific drug-induced sleep endoscopy findings that are associated with better or worse outcomes, and your findings are associated with better outcomes.
Gregory A Tripp Sr. says:
As I prepare for my DISE. I am reading all I can and becoming familiar with the terminology. So what am I hoping for…? That I do not have complete collapse of the pallet? Please tell me what the findings would be if I were to be a PERFECT candidate for Inspire. In other words, what you do not generally like to see as a result after DISE and what you would want to see during the examination for a patient interested and hoping that the implant stimulator will be a good to great solution to their sleep apnea. Thank you and my biggest worry…I will hate (get used to I guess) that big pace maker looking thing bulging out of my skin. I may never walk around with my shirt off again…perceived future. Mr. Tripp, Augusta, GA
Dr. Kezirian says:
Patients who have their tongue as the key cause of their airway obstruction did better with Inspire than other patients, so that might be the “best” finding if you were wondering only about Inspire. Keep in mind that there are other surgical treatment options. As for your other point, the pulse generator (pacemaker) is definitely there and noticeable, but most patients say it is much smaller and less visible to others than they would have expected.