Over the past 15-20 years of my own career, research and experience have dramatically improved results of sleep apnea surgery. For example, we have recently published an international research study showing that drug-induced sleep endoscopy can guide the selection of procedures and whether someone is a good or less-ideal candidate for surgery. In spite of these and many other advances, important questions remain unanswered. One of these questions is whether patients that do not do well after one surgery may respond to additional surgery. I have written previously on this blog about the fact that a sleep apnea surgeon may perform the same procedure on every patient, while results can be much by using newer procedures and better evaluation techniques like drug-induced sleep endoscopy that allow a sleep apnea surgeon or snoring surgeon to choose the right surgery or combination of surgeries for a specific patient.
In spite of these advances, studies have asked whether patients who have not responded to one sleep apnea procedure do as well as those who have never had sleep apnea surgery. There are a couple of reasons why previous surgery could be associated with better or worse outcomes. These reasons have to do with the various reasons that obstructive sleep apnea occurs, ranging from the anatomy of their head and neck to the control of their breathing patterns, how easily they wake up with blockage of breathing, and how the muscles surrounding the throat become more active as the space for breathing in their throat narrows.
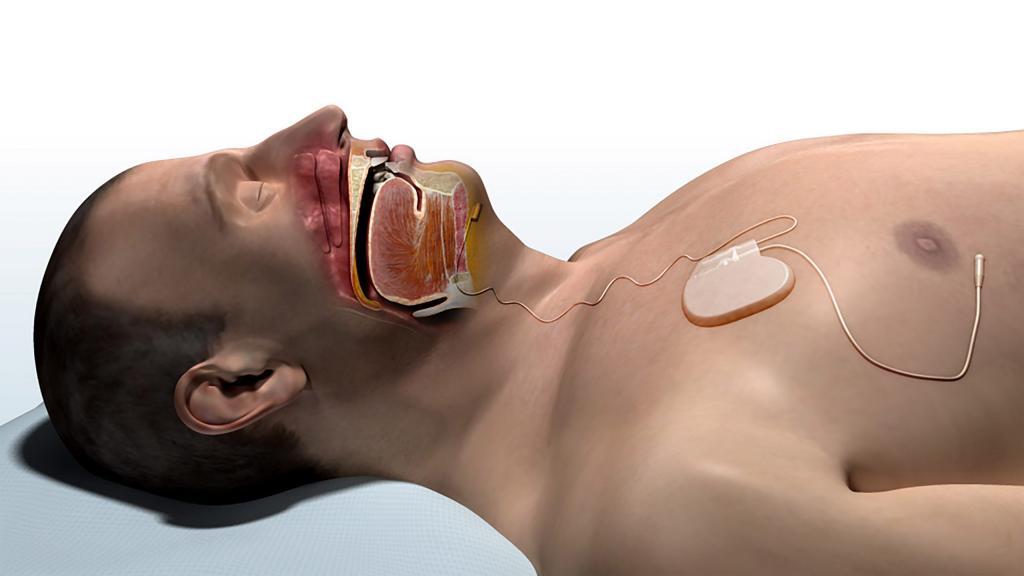
Our group’s research on Upper Airway Stimulation
In order to understand more clearly the outcomes of Upper Airway Stimulation, the company that manufactures the device (Inspire Medical Systems, Inc.) is sponsoring two studies that include multiple major sleep apnea surgery centers around the world. We are participating in both studies. I recently led an examination of data from the Adherence and Outcome of Upper Airway Stimulation for OSA International Registry that examined the question of whether previous sleep apnea surgery was associated with outcomes of Upper Airway Stimulation. This paper was recently published online in the journal Otolaryngology – Head and Neck Surgery.
Among almost 300 study participants, we measured the response to treatment in a couple of ways based on what is called efficacy. We had the following conclusions:
- the clearest result was that there was no clear association between outcomes and previous surgery of any type, previous surgery of the soft palate, or previous surgery of the Palate Region, or previous surgery of the Tongue Region
Two additional findings were not proven statistically but were interesting potential associations that would require a much larger study to evaluate in more detail. Fortunately, the ADHERE Registry continues to enroll study participants and collect data, so we will be able to examine them more completely ni the years ahead.
- those with body mass index lower than the study’s average (29.1 kg/m2) may have a greater chance of response if they have had previous palate surgery
- those with body mass index greater than 29.1 kg/m2 may have a lower chance of response if they have had previous surgery of any kind
The bottom line: if CPAP has not worked well for you, we can help!
Often I hear of patients who have undergone surgery without achieving good results. They think that sleep apnea surgery does not work. This is disappointing. Patients who do not tolerate positive airway pressure therapy (for example, CPAP or BPAP) well should consider options, including surgery. This study showed that patients may be excellent candidates for Inspire Upper Airway Stimulation even if they have not responded to previous surgery. What I tell colleagues in medicine and patients all the time is that we are here to help patients who have not done well with CPAP. We do not give up on patients and believe that a careful evaluation can define the best plan that will work for each patient.
I look forward to continuing to work with this study and other similar research efforts as we move forward in treating obstructive sleep apnea.




6 + 1 =