Inspire Medical’s Upper Airway Stimulation technology is a powerful (no pun intended) addition to the array of options for individuals suffering from obstructive sleep apnea. As a surgeon who implants this therapy, I see patients (whether my own or those coming for a second opinion) where Upper Airway Stimulation is not working well. While there are no magical solutions, it is clear that a careful, thorough approach can often lead to major improvements. Here are some of the steps to take when patients have persistent obstructive sleep apnea after being treated with Upper Airway Stimulation:
1. Do Not Give Up
Treatment with Upper Airway Stimulation is a process. The process takes a few months, starting with the preoperative evaluation and including the implant surgery, activation and adjustment of the system. It can be frustrating to go through this processand not have a perfect result. The important thing is not to give up. Improving results requires everyone to keep moving forward, figuring out why the therapy is not working and coming up with a plan to address the issues.
2. Troubleshooting
There are a number of reasons why Upper Airway Stimulation may not be working well enough. The first step is to collect data from the patient, bed partner, device itself, and the sleep studies done with the system activated. Identify the source of the problem and develop a plan to address it or learn more. When I have encountered unusual issues, I have reached out to the Inspire team. I have been so impressed with their dedication and insight that has helped to resolve issues or overcome obstacles that patients are facing.
3. Awake or Sedated Titration
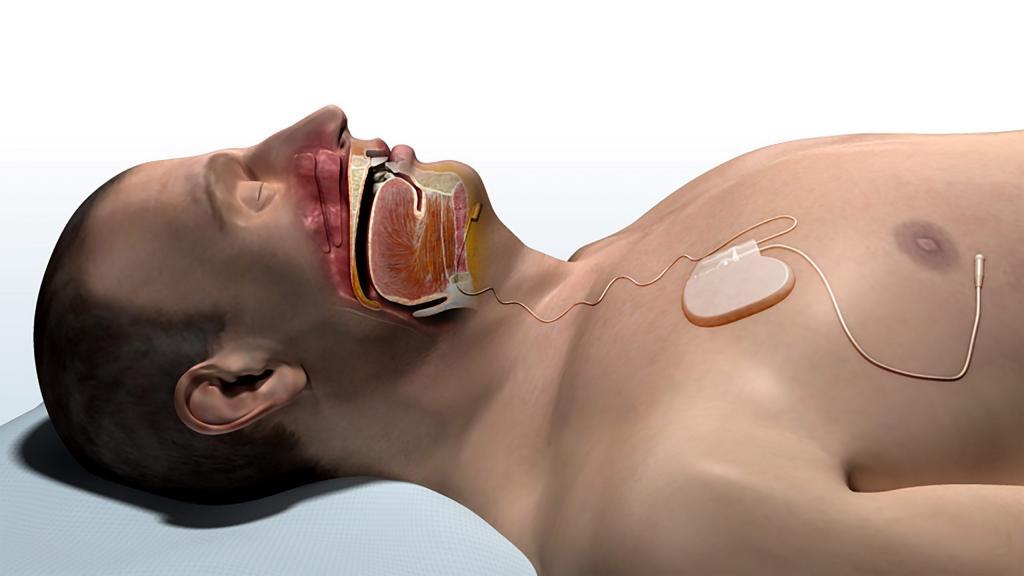
Often everything is functioning properly and the patient is tolerating therapy without not having resolution of their sleep apnea. In these cases, a change in the electrical settings of the device can be helpful. Upper Airway Stimulation includes a stimulation lead that has 3 electrical contacts placed on a portion of the nerve that controls tongue movement (hypoglossal nerve). The system typically delivers the electrical stimulation in a certain manner, using the three electrical contacts with a specific combination of positive and negative settings on the contacts to produce an electrical field for nerve stimulation. Some patients benefit from an adjustment in these settings to modify the electrical field of stimulation if this can move the tongue forward in a more favorable way. The goal is to open the space for breathing not only in the Tongue Region but also in the Palate Region; sometimes a change in the electrical configuration is all that is needed. This exploration of changes is often first done while a patient is awake in the office but can be done under sedation using the technique of drug-induced sleep endoscopy.
4. Consider Additional Treatments, Including Surgery
Treating obstructive sleep apnea often requires a combination of therapies. While the majority of patients have excellent results with Upper Airway Stimulation alone, in many cases another treatment can be added. The other treatment can be something as simple as positional therapy (avoiding sleeping on the back), or it can be another surgery.
The surgeries that can be combined with Upper Airway Stimulation range from a revision of the Inspire system (generally to move the stimulation lead) to adding surgery for the Nasal Region or Palate Region. I have written previously about work presented at the 2018 International Surgical Sleep Society meeting in Munich about good results for soft palate surgery performed in patients treated with Inspire who had incomplete resolution of their sleep apnea. Currently, I have a couple of patients who are considering soft palate surgery and another who would benefit from repositioning of the stimulation lead cuff.
The Bottom Line
The bottom line is that whenever something does not work as well as we would like…find out why and develop a plan to address it.




Terri Bly says:
If it’s primarily the tongue that falls back who does have a deviated right nasal blockage as well; would you recommend first trying less invasive step by trying the Dental appliance? Can you also go over the procedure of what the inspire process is? I’m primarily concerned with the connection of Thank you. The other palate procedures were explained very well.
Dr. Kezirian says:
You should see someone who deals often with obstructive sleep apnea. You should have a formal examination and discussion of your options.
DAN FAUST says:
please help me , i need to sleep and cannot , i have tried several sleep machines and need help. please , please help can you contact me about the tongue stimulation implant. daniel faust 989-304-6400
Dr. Kezirian says:
To schedule an appointment with me, please call our office. We can discuss the array of treatment options, including possible surgery.
Greenbaum Robert says:
Your thoughts on Inspire for position induced apnea (almost 100% when on my back).
My AHI is in the 7-8 range.
Dr. Kezirian says:
I assume that you are not able to use positional therapy (avoiding sleeping on your back) through the entire night. If your AHI is in the 7-8 range, you likely would not qualify for insurance coverage for Inspire. However, there are many other options, whether CPAP, surgery (there are many other procedures), or oral appliances.
Dr. Kezirian says:
Of note, you may very well be covered for these other treatments even though your AHI is not dramatically high.
Brian says:
Can an MMA be done after Inspire implantation?
Dr. Kezirian says:
Yes it can.
Clair Coy says:
My husbands inspire device is not working. Is there a way to trouble shoot it without having to surgically go check it out. Remote engaged. Shows green. Nothing happens. He is on day #5 of using. Last 2 nights it’s not working.
Dr. Kezirian says:
I would speak with your Inspire center. There are numerous potential things that may be occuring. It may be that it needs to be turned up a little.
Michael Giannico says:
I have had the implant for roughly 18 months. I am noticing that I feel it less and less. At this point if I wake up in the middle of the night I don’t need to pause it because the pulsation really isn’t noticeable and i can go right back to sleep. Is this normal? Does the stimulation ‘strengthen’, for lack of a better term, the muscle at the base of the tongue? I understand the stimulation is on the base nerve however as I understand it tightens the muscle. Just like regular exercise strengthens muscles, does this stimulation do the same thing? I still sleep very well, no afternoon tiredness and according to my wife I still snore but do not stop breathing.
Dr. Kezirian says:
You should definitely discuss this with your treating center. It is common for patients to become more used to the stimulation, such that it is not as noticeable. However, you should still notice your tongue moving just as much.
If it is not providing as much movement of your tongue, that may require some further evaluation. You can also just increase the level of stimulation yourself to see if you get even more benefit.
Eric Mullins says:
I feel like the back of my throat closes up, even when the tongue pulses forward, especially when I end up on my stomach (which I can’t seem to help). Scan the therapy make the tongue larger (like it’s exercising all night long). I am noticing more restless nights.
Dr. Kezirian says:
Enlargement of the tongue with nerve stimulation like this has never been shown to increase tongue size. Some people wonder if it might reduce the size of the tongue if it helps with swelling of the tongue or if there is some burning of fat in the tongue (although both of these have never been shown or examined). The next step for you is to see an Inspire team to learn more about why it is not working well for you. Often the cause is that the soft palate (roof of the mouth) is not being pulled forward enough to open the space for breathing there, but only a formal evaluation in person can determine the real reason for your restless nights.
John Manning says:
I just got activated a week ago. Can’t raise the amplitude above 3 (of 10) without discomfort. Could you tell me roughly what the average amplitude might be for the Inspire to be effective? Thanks very much. John Manning
Dr. Kezirian says:
It varies widely from one patient to another. You should definitely be in contact with your center to ask these excellent questions.
Marco Calderon says:
I had inspire surgery done last week. I have slurred speech and trouble swallowing food since then. I have been putting chicken soup in the blender since my surgery and have trouble still 6 days after speaking clearly. Have this happened to patients in the past and how long should I realistically expect to fully heal?
If this discomfort consists is it correctable or will heal on its own?
Dr. Kezirian says:
You should remain in contact with your surgeon, but it sounds like you may have some weakness of the nerve controlling tongue movement (hypoglossal nerve). This can happen after surgery and resolve completely on its own over time. The length of time for healing is not predictable, so you should continue to be followed by your surgeon.
C Wilson says:
Dr. Kezirian,
• I had the Inspire surgery in Florida in 2020.
• The surgery was perfectly executed and the surgeon, sleep doctor, and Inspire rep have made every effort to ensure correct settings.
• I have been trying to fall asleep with 20, 45, and 25 minute lead times before the first “zap.”
• Unfortunately, I don’t think I can ever be compatible with this system because I can only achieve a very shallow sleep up to the start of the tongue control.
• I actually think I had not yet fallen asleep, but my sleep partner says I snore and gasp constantly (my sleep study established waking 55 times per hour). Therefore I do start sleep and it is almost immediately stopped.
• When my tongue starts to move I am at least awake enough to be irritated by Inspire so I become fully awake noticing all of the zaps.
• I reset the remote and try again, but every attempt is the same.
• By 2 or 3 am I turn it off and switch to CPAP (I can’t use Bi PAP for roughly the same reasons). After 14 or so days of this, I am essentially a zombie and I just shelve the Inspire until the next doctor’s appointment.
• The Inspire rep and my doctors have tried to address my dilemma, but since Inspire does not start immediately like CPAP, they seem to be misunderstanding my complaints as “Inspire is irritating” rather than I cannot fall asleep before it starts.
•They keep saying to keep trying because there is an adjustment period.
• The docs say that they are not used to my type of apnea and that all of their other patients can get to REM sleep before Inspire kicks in.
• These medical professionals are completely qualified, but they continue to step around my incompatibility with Inspire and keep tweaking the jolts.
What should I do?
Dr. Kezirian says:
You should keep working with them while also trying to understand for yourself whether a longer delay in the start time would be helpful in allowing you to fall asleep. We have removed a couple of devices because patients could never get comfortable.
Kim Saghy says:
If there is a reason to remove the device, why aren’t the wires removed as well and does insurance pay for the removal?
Dr. Kezirian says:
The whole system would be removed, and insurance should cover this.
Lisa says:
I just want to encourage those posting here to be patient and persistent! Some have said ‘it’s a marathon, not a race’ and I agree. Inspire has been wonderful and reduced my OSA tremendously. But it wasn’t overnight, I ran into setbacks, and was occasionally discouraged. I urge you to contact your Inspire rep for help! Mine has been awesome. Also contact your Inspire doctor. There are many adjustments that can be made to your device, and hopefully some of those will make things better for you. Wishing you all great sleep! 🙂
Carole Nazarian says:
I have Sleep Apnea, but not able to tolerate the C-Pap. Now researching the Inspire approach. My problem is not being able to FALL ASLEEP (along with staying asleep) and wonder if Inspire helps this problem.
Pls. advise.
Carole N.
Dr. Kezirian says:
Inspire can help with this, but our experience is that Inspire may NOT be the right option for people with substantial insomnia. Your trouble falling asleep and staying asleep may prevent you from getting comfortable enough with Inspire to have it work well for you.
Forrest McFeeters says:
I have just gotten the device activated about a month ago. My wife says that my snoring is pronounced but I am not having apnea events. After some trial and error, I find that I get the most relief on a setting of 4/5. However, there are nights where I wake up consistently around 3:30am. I try to pause it and then fall back to sleep but can’t, then I just put on my CPAP and sleep through the rest of the night. I don’t have any lingering daytime symptoms of sleepiness but I can tell that I’m not as “awake” as when I use my CPAP. Increasing the setting would be more uncomfortable for me as I think I’m at the limit of my tolerance at a setting of 5. Is the thinking that I should remain at 4/5 until I start to see consistent sleep through the night? Also, if I know that a pressure of 9.6 on my CPAP is where I get the most relief; is there not any information I can turn to that will let me know what the best setting is that I should use on the Inspire remote based on that pressure setting so I don’t have to do so much exploration? I’m sure the data is out there.
Dr. Kezirian says:
It is great to see that you are already experiencing some improvements so soon. You should remain in contact with your team. There should be an overnight sleep study where they will check what settings might work best for you. This is called a titration study and is usually done at 2-4 months after implantation.
Rick says:
My device was implanted in Oct. 2020. A sleep study was done and the Inspire rep told me they were seeing an artifact on the lung sensor so they shut if off and would contact me in the future about what they’ll do. I don’t notice much help with the device. I have told them since the beginning that 2 things are very wrong–1. the sensor is not timing the pulse to my breathing and 2. my tongue is being pulled backward instead of pushed forward. Months ago they said that was not abnormal but now they’re saying it is??? What the heck?? To me it seems counter productive to have the tongue move back towards the throat?? Your opinion as to what is going on.
Dr. Kezirian says:
There could be a lot of things, but you shuld continue working with your Inspire team. Clearly, the system should move your tongue forward, so the stimulation lead in your neck might need to be repositioned (with a surgery) if it is not doing that.
William Johnson says:
I got the inspire implant about two months ago. I must be a poster child for inspire because of the fantastic results I have experienced. I sleep soundly thru the night feeling none of the side effects I have read about. I am on level 10 of the second level of settings. I do notice some small movement of my tongue but only when I turn it on at night. I do not feel anything while I’m asleep. I wake up incredibly refreshed and hit the day strong mentally and physically. I can say the implant is a mericle of modern medicine, and has changed my life. I don’t know too much about the alternatives but from all I’ve read there’s nothing that works as well as the inspire. I know that I was largely
unaware of just how much my sleep apnea was effecting my overall being. I sleep tested with 75 incidents of stopping breathing in one hour, that’s bad. I lost 60 pounds to become eligible for the inspire implant and my sleep apnea went down to a level that was acceptable to proceed. I’m 71 by the way, so it’s probably not to late for you to investigate inspire with a qualified doctor. Probably after my daughter’s birth it’s the greatest thing that’s ever happened to me.
Dr. Kezirian says:
I am so happy that you have had such a great result.
George Boardman says:
I’m brand new also. One month into activation. I’m at level 5 so far. 1st night 5 hours of uninterrupted sleep! Fantastic! Since then not so much. I take 0.8mg of Flowmax around 6pm each night and of course I’m up going to bathroom 2 or 3 times. I do feel inspired by your comments and to be patient. I’m 76 yeat old male and patience is not my strong suit. Thanks for being on here and your encouragement.
Tom says:
My ENT has completed my sleep endoscopy and declared I am an excellent candidate for Inspire. I am very excited and going through final authorizations before scheduling surgery, but have some questions around lifestyle impacts. I am an active yoga practitioner so require a very wide range of motion, and I participate in competitive shotgun sports and can not implant on the right pectoral muscle due to gun placement and recoil effects. My surgeon does not want to implant on the left side and suggests locating the device on the right side closer to my breast plate where it may be highly visible. Does anyone have information on alternative placements and range of motion restrictions? Can this be placed in the armpit or side of the chest?
Dr. Kezirian says:
I do not have specific experience with implanting it more medially on the right side. The typical thing would be just to do the left side, as this is done often. You should involve the Inspire representative, who can speak with colleagues and learn from the experience of other surgeons too.
Dee says:
It will soon be a year since I had the Inspire system implanted. My main problem is insomnia. It takes me several hours to fall asleep and then I wake up frequently throughout the night. I am aware of Inspire enough that it is very annoying. Some nights I don’t even use it because I simply don’t want to deal with it. That in no way means that I will sleep….in fact…..I probably won’t sleep. But at least if I don’t have it on I don’t have to deal with it. My doctor and the Inspire reps try new configurations each time and they tell me it is a process but frankly I am very discouraged. My doctor has tried various meds to help me sleep but nothing has worked. I feel doomed!
Dr. Kezirian says:
Significant insomnia can make getting comfortable with Inspire difficult. We have stopped implanting patients with substantial insomnia because we have seen a couple of patients like you (one implanted by us, others at outside centers). Some studies have shown that Inspire treatment can improve insomnia symptoms, but our results have not been great.
Tina says:
I’ve had my Inspire for about 6 months now. My doctor said
” Your AHI was 38 (severe OSA), and now it’s 19 (moderate OSA). If possible, I’d like to see us get that number a little lower.” I was able to gradually move my voltage up to ten but started noticing my tongue would feel a small burning sensation shooting down the right side of my tongue. Then, I would wake up with my tongue feeling more raw and painful each day, like I scalded the right side of my it on hot coffee. My doctor brought me in and did some adjustments which seemed to help for about a week , then, the raw burned sensation has moved to over the top of my tongue. I had to forgo my Inspire for a few nights to let it heal. The Inspire has helped me a ton though, my spouse says he doesn’t hear me snore or struggle for breath anymore. My CPAP machine is almost too painful at the level I need because it feels like it’s popping my ears from the air pressure. Have other Inspire patients run into this and can it be fixed? I don’t want to give up on this device and keep imagining I’ll have to spend the rest of my life rotating between burning my tongue on the Inspire and popping my ears on the CPAP to let my tongue re-heal.
Dr. Kezirian says:
You should not be having tongue pain unless your tongue is rubbing on sharp edges of your teeth. The electrical stimulation should not affect the nerve for sensation (touch and taste), so I am not sure if a different adjustment would be helpful.
Mike says:
I’ve had Inspire for almost two months. Before I got Inspire I was told I had hypertrophy of the tongue base and that the device would help that. Even while awake, I feel my tongue base touching the back of my throat and get winded during normal walking and stairs etc. When my device turns on I feel an increase of pressure in the tongue base area. I haven’t been able to get above level 5 in the last 6-7 weeks. I bumped up to level 6 last week and slept horrible. To me it feels like my tongue is being moved by the stimulation in the wrong direction narrowing my airway instead of opening it. Can Inspire manipulate my tongue enough to overcome the hypertrophy? Have you seen any cases where removing excess tissue from hypertrophy is beneficial?
Dr. Kezirian says:
You should speak to your Inspire team. First, it is still early at just 2 months after implantation. Second, there can be some changes in the way the electrical signal is sent to your nerve. Third, it is possible that the stimulation is happening on a place along the nerve that stimulates various nerve branches that could move the tongue backwards instead of forwards. This could need a revision surgery, but the electrical adjustments can often help quite a bit.
Inspire therapy is not perfect, but it should help in cases of tongue hypertrophy. However, it would not be expected to change the tongue hypertrophy; it just moves the tongue forward so that it is less likely to block your breathing. In general, one would be cautious about the various treatments to reduce the size of the tongue physically, but those could be performed if various changes do not work.
Dee H says:
I wrote in June about having insomnia and having a lot of trouble with my Inspire. You responded that you don’t even implant people anymore with significant insomnia. I am still STILL dealing with this issue. In fact my doctor the last few months has been solely trying to find the right meds to help me sleep first and then to address the device. I have not seen the Inspire reps for months. Obviously there has been no sleep study yet so no one even knows if Inspire is helping me at all. The quality of my life in this area is horrible. I am seriously thinking of having it removed. Are there risks snd if so what are they?
Marly V says:
My partner had the Inspire inserted in January. He just left his second appointment and they told him the data indicates it is not working for him (although the snoring has stopped) they aren’t scheduling a sleep study, told him he doesn’t need to be seen by their clinic anymore, and a Inspire rep will be in touch…After thousands of dollars and being told he was the ideal candidate (unable to keep the CPAP on at night, 35+apneic episodes/hr, and otherwise healthy) we are devastated. Is it really time to throw in the towel already? I worry about how he is going to ever have quality sleep and for the longevity of his life. They gave us not one word of hope…any thoughts or recommendations? Thanks
Dr. Kezirian says:
I would also be devastated. This is not the time to give up. You should check in with the Inspire representative to understand why this was their conclusion. The system is either not turning on properly, not placed correctly, and/or not the right knd of sleep apnea. If there are no real answers, I would go to another Inspire center to sort out what might be happening. We see patients who have not had full response with Inspire therapy – from our center and others – and we do not just give up. We figure out what is going wrong and take it from there.
Wisconsin Ron says:
My identical twin had the inspire device implanted a year ago. I had my first PSG last week and I have confirmation of what my wife has been telling me for years, I have Sleep Apnea. Please explain to me how your team (PSG lab, Inspire Rep, Implant Surgeon, Nasal/Pallet/Tongue Surgeons & Patient) works together to help patients achieve their best possible sleep quality in complex scenarios where both surgery and a stimulation implant are needed to achieve the best possible sleep quality. I have retired to the west coast and am looking for a sleep team.
Dr. Kezirian says:
You can learn more about this on my website at https://sleep-doctor.com/surgical-treatment-overview/upper-airway-stimulation/. In short, I see many patients who have not achieved ideal results from other centers. My research has focused on using all available tools to select the best approach for each patient and solve complex scenarios. Please contact our team (I am actually in the midst of changing my contact information on my website to reflect my move to UCLA starting in July 2023.
peggy says:
I have the Inspire device, implanted over a year ago. I recently lost 50n pounds and I have been told by a few doctors and nurses that my neck size is so small there is no way I can still be positive. I am having a Sleep Study performed next week to see if in fact I am still positive. The moving on my tongue has gotten to rubbing against my teeth which has caused my tongue to bruise….I see a dentist next week as well……hopefully one or the other will go!!!
Dr. Kezirian says:
It sounds like a repeat sleep study (without any treatment, including leaving your Inspire system off for the night) would be a good next step. Of course, you can always evaluate whether your sleep is any different if you just leave your Inspire system off for a night. If you do not have any sleep apnea, there should be no changes with the Inspire system off vs. on. Lastly, with your weight loss, you likely can turn down the intensity of the Inspire stimulation, but you should discuss this with your Inspire team. This may help with the tongue rubbing against your teeth.
Glenn Varner says:
I’ve had my device activated for a little over a month now. When I turn my device on at night, everything works as expected. However, I wake up a few hours later and my tongue doesn’t seem to be moving. If I pause it, it does make my tongue move forward, but to a lesser degree and after 5-10 times, it just feels like my throat is wide open, but the movement of my tongue ceases. Could my tongue be held in the stimulate position constantly even though the system is providing a pulse signal? It really feels like my tongue is moved forward at the base as if it was in that contractive mode
Dr. Kezirian says:
This is something that you should definitely discuss with your Inspire team. I have not heard of something like this before. The fact that you are waking up may throw off the signals that the system uses to guide the timing of the stimulation. Regardless, this should be discussed with your team.
George E says:
I have severe sleep apnea. CPAP and BiPAP did not help me. My insurance denied Inspire for two reasons. They claim it is still classified as an experimental device. I recently did a home sleep study waiting for the results for improvement to API wearing oral appliance recently fitted by a dentist. Hopefully in the future I can revisit Inspire again for consideration.
Barry Hogue says:
Hello, I have moderate apnea with an AHI of 18 and as of a week ago I have been unable to sleep well due to when I drift to sleep I begin snoring and jerk myself awake. It seems as if my soft palate is vibrating and causing this snore. If i get inspire, does it also open up the area weekdays the soft palate is to prevent this snoring? It should be great to have both of these issues finally fixed.
Dr. Kezirian says:
Inspire is programmed to start after someone falls asleep, in almost all cases. The result is that it will likely not address anything happening as you drift off to sleep. However, you should discuss this with your Inspire team.
Carl Marte says:
I’ve been implanted with Inspire, but now I want an epiglottopexy and tongue base reduction. Is it possible to do the tongue base reduction with no negative effects on the inspire lead?
Dr. Kezirian says:
You should speak with your surgeon about this and also ask why you would want or need these other procedures. In general, you want to be careful using monopolar electrocautery after an implant, especially if you are operating near any of the components.