I see patients all the time who are coming in for the first time to see someone for an evaluation of snoring and possible sleep apnea. After I explain what sleep apnea is and order a sleep study, they almost always have a few questions:
- If I have sleep apnea, what are my treatment options?
- You mentioned this mask and treatment called CPAP. How can you expect me to sleep with that mask on my face?
- Can’t we just do surgery and take care of the problem right away?
The answers I give are those that I offer to my own family and friends. For patients with moderate to severe sleep apnea, CPAP remains the first-line therapy. Patients who do well with it love it. I had a close friend visiting me last month who offered to be on any public service announcement I might have because he has had such a dramatic improvement with CPAP and has been able to use it comfortably all night, every night.
On the other hand, multiple studies have shown that about half of all patients with sleep apnea are unable to tolerate positive airway pressure therapy (such as CPAP, BPAP/BiPAP, or APAP/AutoPAP). Most of these have focused on individuals who wore CPAP during at least part of a night and then indicated they would be willing to use it at home. These studies ignore those who find CPAP completely intolerable and refuse it immediately, making the true estimate of difficulties with CPAP a little higher than most studies would suggest.
What happens if you hate CPAP?
A study published in the November 2015 issue of the medical journal Otolaryngology–Head and Neck Surgery examined over 600 patients who were newly diagnosed with obstructive sleep apnea after a sleep study at the Cleveland Clinic over a 2-month period in 2010. Almost 17% of the patients refused CPAP immediately after their initial exposure to it and never obtained the equipment for use at home. Of the patients who did agree to use CPAP, about 60% were still using it at their last follow up (in some cases 3 years after the initial diagnosis), although that still only represents 42% of the total group. For the 58% who did not do well with CPAP after it was recommended, some (about one-fifth) were referred either to a sleep medicine specialist, otolaryngologist–head and neck surgeon, or dentist. However, that meant that almost half (46%) of the entire group of patients newly diagnosed with sleep apnea were unable to tolerate CPAP and did not receive a referral to a specialist to assess their treatment options. Their conclusion was that there are gaps in the management of patients with sleep apnea who fail or refuse CPAP.
Obviously, there is no concerted effort to leave sleep apnea patients without treatment. Some of the patients in this study without CPAP or a documented referral must have seen a specialist at some point in time, even if outside the Cleveland Clinic system. However, some of these patients with referrals probably did not have the chance to evaluate the full spectrum of treatment options. Overall, it is very possible that almost half of all patients with sleep apnea go untreated because they fail or refuse CPAP, and this is the first study to document how common this situation may be.
What does this mean for sleep apnea treatment and sleep apnea surgery?
We know that we in sleep medicine must do better in following up on patients with sleep apnea, regardless of what treatment they undergo. I personally tell all of my patients, even those with fantastic results after sleep apnea surgery, that they should return to see me if any aspect of their sleep apnea returns, whether it is snoring, poor sleep quality and all of the symptoms like sleepiness and fatigue, or health concerns like high blood pressure that is difficult to control with medications. From their initial visit, we also review the full range of treatment options for sleep apnea and discuss whether each is a reasonable approach for them.
Patients share their experiences with sleep apnea surgery, including this one on CBS News
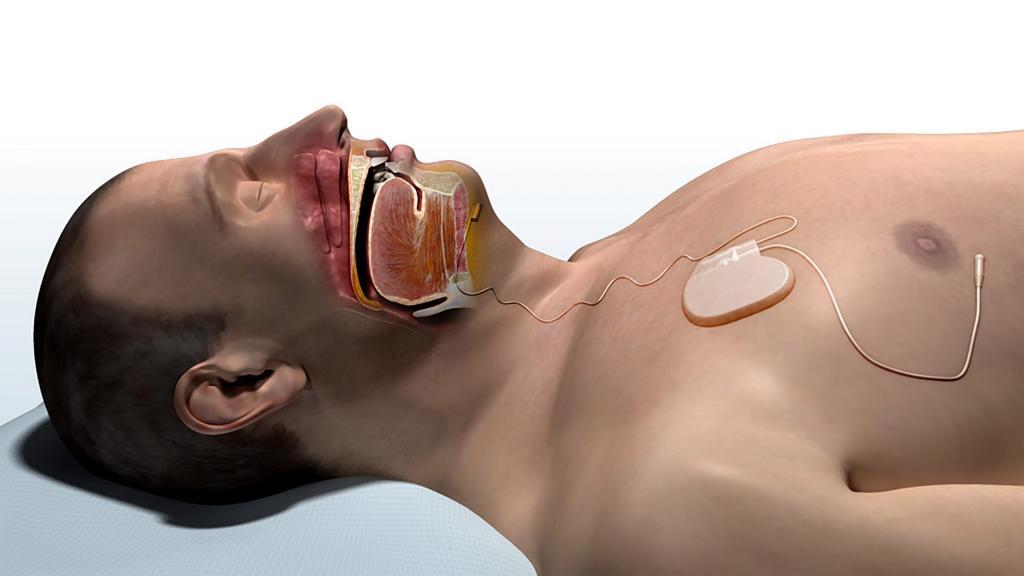
When it comes to sleep apnea surgery, we in the field are making a concerted effort to train surgeons in the wide array of surgical procedures for sleep apnea and how we choose from among them. The recent development of the Upper Airway Stimulation system (shown below) has fostered collaboration between surgeons and sleep medicine physicians that should enhance our work together to maximize outcomes for patients. Of course, the best people that spread the word about the benefits of alternative treatments are our patients. This past week, one of our patients was featured in a CBS News segment about Upper Airway Stimulation and the work we are doing at Keck Medicine of USC. I thanked him for taking the time to share his experience and benefit others.




Suzanne says:
Being the spouse of husband’s cpap so-called treatment. ..I refuse it! It has interfered with every aspect of our lives, including the cat .The machine freaks me out and looks like and sounds like a life -support machine that belongs in a nursing home or hospital.
The machine is competing with me and receives precedent over me. The machine requires gentle care ,paid attention to, cleaned and lovingly cared for and about.
It is intimate and sleeps with him kissing him on his mouth.
I will NOT sleep with a mistress so he now sleeps in another room with his new mistress.
You people are neglegent to not address spouses negative reactions to this invasive machine. It’s horrible! I’m going to have to travel to all the fun adventures we were planning because I will not share those experiences with a machine.
Dr. Kezirian says:
I understand your concerns, but at the same time many spouses report that the hum of the machine is better than the irregular pattern of snoring and choking. Regarding the concerns about intimacy, obviously CPAP can interfere with intimacy because it is hard to kiss someone when they are wearing CPAP. However, I would try to think about the CPAP as similar to other things that people wear to bed on their face like eye masks, ear plugs, and moisturizing cream. I clearly perform surgery in many patients who cannot tolerate CPAP, but usually it is the patient themselves who has problems. Most spouses are very happy to see a more-energetic (and perhaps less irritable) person who has had a good night of sleep if the patient can sleep comfortably with CPAP.
Robert says:
The CPAP is frequently described as a “Cure” for Apnea. That is like saying the Iron Lung ( https://en.wikipedia.org/wiki/Iron_lung ) is a cure for polio. It is a machine that manages symptoms of a medical condition. Patients who can not tolerate the machine are considered not “Compliant,” as if the source of their inability to breathe properly are their fault. We need better (and more competent) doctors and surgeons to address the underlying causes of Obstructive Sleep Apnea rather than blame those who suffer from it for the failure of treatment.
I am thankful for my CPAP for keeping me alive, just as I would be thankful for a feeding tube while in a coma. However, I would prefer to breathe on my own just as I would prefer to eat on my own. Nobody wishes for a colostomy bag or a catheter. Nobody hopes to be plugged into a dialysis machine. These are not cures. This is management of a condition. Please stop treating CPAP (and similar treatments) as cures, and please stop demonizing those who suffer from the treatment while waiting for someone to resolve the underlying issue. No doctor worth a degree would recommend “Stuff your underpants with toilet paper” as a cure for diarrhea. Why is “Stuff your nose and mouth with compressed air” considered a “Cure” for an inability to breathe properly?
Dr. Kezirian says:
Thank you for your comments. You correctly point out that we need to learn more about the causes of obstructive sleep apnea. I cannot say I agree entirely with the analogies you present, but you are also absolutely correct in that CPAP is not exactly a cure. It is more of a good way to manage obstructive sleep apnea for many patients–although certainly it does not work for many. The analogy that I like to use relates to diabetes or high blood pressure. Medications, diet, and exercise can manage these conditions (and sometimes resolve them), but they are not what we would refer to as a cure. Either way, I hope you have been able to find success with CPAP or can see someone like a surgeon who can discuss potential options if CPAP is not working well for you.
Joanne Hurdle says:
Hello
My partner has been diagnosed and has been struggling with the CPAP mask for a few months. He is unable to sleep with it on and suffers claustrophobia. Within a few moments the mask is torn off and he gasps for air in panic. Because of this he is now suffering more than he ever did before being diagnosed and is definitely on the edge of pure exhaustion or a breakdown. We now sleep separately and he says the mask has ruined his life. While I appreciate the mask can actually save his life surely there are alternatives for patients like him who cannot use it. I have joined a support group but we are desperate for help as soon as possible. The Nurse at the hospital just told him ” good luck with speaking to the consultant as there are thousands who need help” which wasn’t good to hear. Please advise what the eligibility is for the operation I have heard about. Thank you so much for any help you can offer. Kind regards Joanne Hurdle
Dr. Kezirian says:
Your partner is not alone, as this is one reason that patients cannot tolerate CPAP. If he cannot tolerate it, he should discuss it with his health care team. I expect the last thing anyone wants is to make things worse. There are options – including various types of surgery – for a patient who cannot tolerate CPAP. Surgery would generally be covered by insurance for someone like him, so the real question is what kind of surgery would be best and what the expected results might be. I would be happy to see your partner as a patient in the office.
Sue O. says:
I was diagnosed with mild sleep apnea. I’m a female, are 71. My adult medicine doctor ordered the initial sleep study and then I also had the titration study. I had a very bad experience using the test CPAP during the titration night. A CPAP was prescribed for me. However, the other doctor (sleep doc) who read the results and prescribed the CPAP will not see anyone in person until they’ve used it for 3 months. No one ever provided me with education or an in-person visit about sleep apnea. I went to the medical equipment place. After hearing some information about using it, I refused to take it home with me. I feel like I’ve been led around by the nose, with No counseling, etc. I am depressed, sad, and mad.
Dr. Kezirian says:
I am sorry to hear this. It should like you should consider finding another sleep medicine provider. Your adult medicine doctor may have a recommendation.
llz bird says:
I have been diagnosed by my dentist with mild to moderate sleep apnea. I am extremely claustrophobic and always have been. I also get anxiety attacks. I patently refused to wear any kind of mask to bed. I tried once because I really like my dentist, but I have never liked wearing anything on my face or around my head. I don’t even like hats. I don’t wear eye masks to bed. Some glasses even bother me.I struggled to find glasses that did not hurt. Therefore, I think I would rather live what life I have left than be forced to wear a CPAP.
Dr. Kezirian says:
Your inability to wear masks is common. For you, treatment options for obstructive sleep apnea may include conservative measures, oral appliances, and surgery. You should discuss these with your dentist and anyone else providing health care for you.
Jami Hede says:
I was first diagnosed with OSA in the mid-1990s. After I was unable to tolerate CPAP, I was placed on BiPAP. For the next several years. I was able to tolerate it for at least a few hours a night. In fact, my boss Imptoved to the point that I was able to sleep without the device if I slept on my side.
Things changed. I underwent chemotherapy after surgery to remove a malignancy in my female organs. This was successful, but I began to notice a downward decline in my sleep. In fact, things have gotten to the point where I cannot tolerate pressure at all.
Currently, the introduction of even a minimal amount of pressure into my airway results in a complete inability to breathe. The pressure continued to build until I end up ripping off the mask just so I can breathe. This usu as lly happens in less than one minute.
The problem is not the mask. I can tolerate any mask, as long as no pressure is introduced. Ramping doesnt hrlp; even the barest minimum of pressure cannot be tolerated. We tried switching to an APAP machine, with no success.
I have seen five different sleep specialists in the last six years. None of them will consider any other treatment than BIPap. All they do is tell me to try harder, and eventually tell me that they don’t know what to do with me. One told me to go to Mato. but I have no way to get there, let alone mo ey to pay for it.
I’m at my wife’s end. I dont know where to go or how to pay for it. Do you have any ideas*
Dr. Kezirian says:
It sounds like you should see a sleep surgeon. BPAP would be unlikely to solve this problem. It could actually be that the pressure is pushing your epiglottis down to block your breathing completely. Regardless, you cannot tolerate positive airway pressure therapy, and surgery or oral appliances are commonly used in patients like you.