The 2018 Annual Meeting of the American Academy of Otolaryngology – Head and Surgery (AAO-HNS) was held earlier this week in Atlanta, Georgia. It was a wonderful opportunity to share experiences with long-time colleagues and some that I had not met previously. In addition to my presentations related to drug-induced sleep endoscopy, Tongue Region Surgery, and non-surgical treatment of obstructive sleep apnea, there were some interesting presentations related to research. I wanted to write on some of those in this month’s post.
OSA and Cancer Risk
Over the past years, interesting studies have indicated that obstructive sleep apnea is associated with an increased risk of cancer, especially certain types of cancer. Edward Weaver and Sebastian Jara from the University of Washington examined administrative data from United States Veterans Affairs Medical Centers in the United States from 1993-2013. They compared about 100,000 individuals who had a diagnosis of obstructive sleep apnea to similar individuals without obstructive sleep apnea. The research was focused on whether obstructive sleep apnea increased the risk of developing cancer, so they only “counted” cancers that first appeared as a diagnosis at least 2 years after the first diagnosis of obstructive sleep apnea. They found that obstructive sleep apnea was associated with double the risk of cancer (hazard ratio 1.97; 95% confidence interval 1.94, 2.00), with a consistent association across various types of cancer.
This excellent study was important because it went beyond the smaller previous studies and showed the effect in a broader (and larger) group of individuals across over 100 hospitals throughout the country, making it clearer that this association is real. For patients with obstructive sleep apnea, especially severe sleep apnea, the cancer risk is not as important as the association with cardiovascular disease like hypertension, heart attack, and stroke, but it may be another important benefit of obstructive sleep apnea treatment.
Mouth Breathing and Mouth Opening
Dr. Bin Hu from Beijing spoke about the potentially-important effects of mouth opening on obstructive sleep apnea. This study compared measurements on an X-ray of the head and neck called a lateral cephalogram performed with the mouth closed and then the mouth open. Mouth opening – whether because of blockage in the nose or because of the habit of mouth breathing – was associated with narrowing of the space for breathing in the Palate Region and Tongue Region. The effect was greater in those with relatively large tongues, defined as Modified Mallampati Position 3. My own previous research using drug-induced sleep endoscopy, has shown that mouth opening may be one reason that patients do not respond to sleep apnea surgery. The team from Beijing should be congratulated for a well-done study highlighting the breathing through the nose instead of the mouth during sleep.
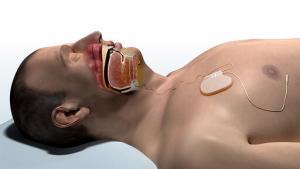
Upper Airway Stimulation and Previous Surgery
Inspire Medical Systems is supporting two ongoing studies related to Upper Airway Stimulation therapy. The Post-FDA-Approval Study is ongoing, but there are some early results from the Adherence and Outcome of Upper Airway Stimulation for OSA International Registry (ADHERE Registry) are available. For patients who do not tolerate positive airway pressure therapy, Upper Airway Stimulation can be used as the next treatment, but sometimes patients have had previous sleep apnea surgery. There are reasons to believe that those with other sleep apnea surgeries would do better or worse with Upper Airway Stimulation. At the AAO-HNS Meeting, I presented research from the ADHERE Registry showing that Upper Airway Stimulation can produce the same results in those with and without other previous sleep apnea surgery. In short, although a patient may not have responded to previous surgery, they may still respond well to Upper Airway Stimulation.
Upper Airway Stimulation and Older Adults
Because obstructive sleep apnea is so common in older adults, there is a large potential group of Medicare beneficiaries who could be treated with Upper Airway Stimulation. The challenge is that Medicare has not issued a clear National Coverage Determination (or even a Local Coverage Determination) related to Upper Airway Stimulation, meaning that it may or may not be covered in individual cases.
Using the ADHERE Registry data, the team at the University of Alabama at Birmingham School of Medicine, led by Kirk Withrow, examined the question of whether adults aged 65 years and older do better or worse with the Inspire Upper Airway Stimulation. Their study showed that, interestingly, older adults actually appear to do better than young and middle-aged adults. We certainly have had some real success in older adults but are currently in a holding pattern while we await a formal Coverage Determination. Hopefully this study will pave the way for an official assessment and decision.




14 − = 11