Palatal advancement (also called palatal advancement pharyngoplasty or transpalatal advancement pharyngoplasty) is performed under general anesthesia in the operating room to treat obstructive sleep apnea. It is performed less often than other types of palate surgery, but it is an important surgical treatment option that may work better in certain types of patients.
During this procedure, Dr. Kezirian removes a small portion of the back of the hard palate (firm part of the roof of the mouth) and moves the soft palate (soft part of the roof of the mouth) forward. This enlarges the space for breathing behind the soft palate. It may be combined with tonsillectomy and other soft palate surgery.
What makes palatal advancement a good sleep apnea surgery?
The goal of the procedure is to increase the size of the airway without affecting normal functions such as breathing, speaking, and swallowing. Most palate surgeries remove or reposition tissue of the soft palate. This surgery is different. It involves a special incision that exposes the back of the hard palate and part of the soft palate. A small portion of the back of the hard palate is removed carefully, and the soft palate is then pulled forward and held in position with stitches placed in a specific way. It does require more dissection, making it more difficult for surgeons to perform, but there is actually often less pain than other types of soft palate surgery.
Palatal advancement opens the space for breathing behind the soft palate (Palate Region) by pulling the soft palate forward. This creates a different kind of opening than other palate surgeries. Relatively few surgeons perform this procedure, but Dr. Kezirian performs it because there is reason to believe it is the right procedure for some patients. Pulling the soft palate forward also pulls on the sides of the throat, which is important for certain types of blockage in the Palate Region (whether shown with awake examination or drug-induced sleep endoscopy).
Palatal advancement was first described 30 years ago, but there were important risks of complications that could result in poor healing. Over time, the procedure technique has been modified to improve healing and substantially lower these risks. These complications include having the soft palate pull away from the hard palate and having a hole develop to connect the mouth with the nasal cavity directly above it (called an oronasal fistula). This can be treated with a special mouthpiece to cover the hole, and fortunately it will often heal completely without the need for additional surgery. However, it is important that surgeons have improved the technique to lower this risk, making Dr. Kezirian more comfortable with performing the procedure in the first place.
For more information about the selection of palate procedures, please see Dr. Kezirian’s blog entry about choosing the best palate surgery for snoring and sleep apnea.
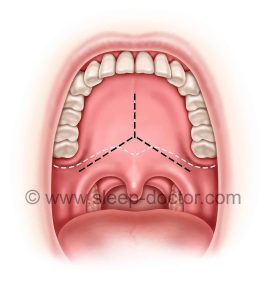
Incision over the soft palate and hard palate (edge of hard palate shown with white dashed line)
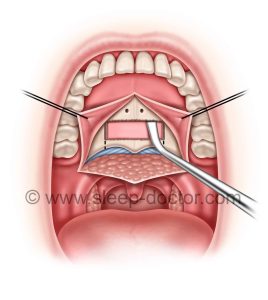
Removal of bone from the back of the hard palate
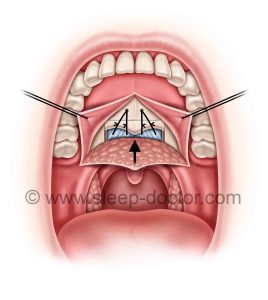
Advancement of the soft palate, using a small piece of hard palate bone to hold it in place
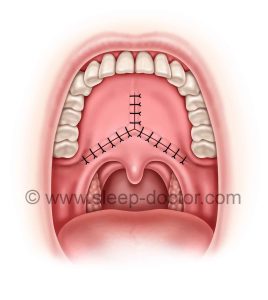
Closure of incisions, with the soft palate advanced
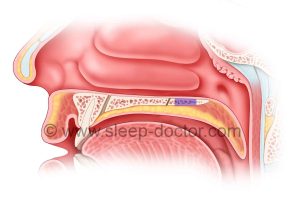
Side view of palate, with shaded area showing hard palate bone removal
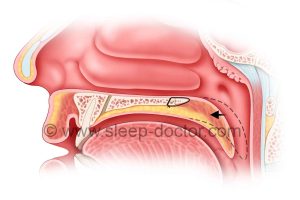
Side view of palate, showing opening of the airway with advancement of the soft palate
RISKS
Bleeding
Palatal advancement carries a risk of bleeding. A major factor in preventing serious bleeding is to avoid the use of aspirin, NSAIDs (such as ibuprofen, Advil®, Motrin®, naproxen, or Aleve®), vitamin supplements, or herbal medications for at least two weeks before and after surgery. If bleeding occurs after surgery, it may require an additional procedure—either in the outpatient clinic or the operating room—to control the bleeding. Please notify Dr. Kezirian immediately if you have bleeding of a teaspoon or more. If the bleeding is significant, immediately seek care in the closest emergency department or call 911.
Infection
Infection is rare but not impossible after palatal advancement. Patients typically receive antibiotics at the time of surgery to reduce the chance of infection and decrease swelling. Patients should not use mouthwashes following surgery because many of these contain alcohol that can irritate the lining of the mouth and interfere with healing.
Fistula
Oronasal fistula is a hole in the roof of the mouth that connects the mouth and the nose above it. An oronasal fistula can form during the healing process after palatal advancement due to poor healing of the lining of the mouth or of the connection of the soft palate and hard palate. With the initial surgical technique described 30 years ago, the risk of fistula was close to 20%. However, two important changes in the surgical technique have been developed over time, lowering this risk dramatically to less than 5%. Avoiding hard foods for the first 3 weeks after surgery is important in all patients, as hard foods can interfere with healing of the roof of the mouth. If a fistula develops, the good news is that it generally heals without needing any involved treatments, but usually a special mouthpiece is required to cover the healing area and protect it during healing. Additional procedures to close the hole may be required, and there is a very small risk that it cannot be closed.
Difficulty swallowing
The palate and sides of the throat are important in swallowing. After palatal advancement, patients may experience two kinds of difficulties with swallowing. Many patients have liquids or food come up in the back of the nose or occasionally through the nose because the soft palate is not performing its normal function to separate the back of the mouth from the back of the nose. This happens in many patients for a brief period (1-2 days) due to swelling in the soft palate and can occur with an oronasal fistula, but it is unusual for this complication to be permanent and significant. The second kind of difficulty with swallowing is that liquids or food may go “down the wrong way” towards the lungs, resulting in coughing as an attempt to clear the material. This can occur due to swelling and pulling on the muscles in the sides of the throat but is usually temporary. It can occur for a more prolonged period, but it is rare for this to be permanent.
Changes in speech
Any operation on the palate and sides of the throat can cause changes in speech, but these changes are rarely permanent.
Throat dryness or feeling of something stuck in the throat
Any operation on the palate can affect the throat in unpredictable ways, and it is possible for some patients to dryness or a feeling that something is stuck in the throat. These are usually temporary, but they can be permanent.
Change in sense of taste or tongue numbness
There are taste buds throughout the mouth, and it is possible that surgery of the palate can produce a change in the sense of taste or tongue numbness. This can be due to the surgery performed in the palate or pressure against the tongue from the surgical instrument placed in the mouth for the procedure. If there is a change in the sense of taste or tongue numbness, usually the damage is temporary with recovery over the course of days or weeks, but the damage can take months to recover or be permanent.
Tooth injury
Operating in the mouth and throat is impossible unless an instrument is placed to keep the mouth open. This is the same instrument used when tonsillectomies are done. Rarely, a tooth may be injured by this instrument, and the risk is much higher if a tooth is loose or decayed prior to surgery.
Continued snoring
Most patients undergoing palatal advancement will also have loud snoring. The goal of surgery is to eliminate obstructive sleep apnea. Usually snoring will improve dramatically if this goal is accomplished. However, many patients will continue to snore to some extent, even after surgery that resolves obstructive sleep apnea completely.
POSTOPERATIVE INSTRUCTIONS
NOTIFY DR. KEZIRIAN IMMEDIATELY IF YOU HAVE ANY TROUBLE BREATHING OR IF ANY BLEEDING DEVELOPS!
Hospital stay and discharge
Most patients stay in the hospital 1 day. The major concerns while you are in the hospital are making sure you are breathing freely, having no bleeding, controlling your pain with oral medications, and drinking enough fluids to have no risk of dehydration. Many people ask if they need someone to stay with them at home. For your safety, you do need someone to stay with you the first night home after discharge. Beyond that, it is helpful to have someone available and checking on you to provide assistance when needed, although they do not have to stay with you 24 hours a day, every day. Planning before surgery (for example, buying milk or nutritional supplements) will decrease the amount of help you need at home after surgery.
Pain control
Like most surgeries, there is pain in the recovery period. However, we want to control your pain to make you comfortable during your recovery. Some people try to “hang in there” or suffer without taking pain medications. Controlling your pain is important for breathing, healing, and being able to swallow enough to maintain your nutrition.
While in the hospital, we will control your pain with oral medications, starting on the day of surgery. You can also hold ice chips inside your mouth to decrease swelling and reduce pain. Although we will use intravenous pain medications if necessary, the goal will be to use oral medications alone because this is what you will use when you go home after surgery. You will not receive a prescription for pain medications before surgery, as we will send you home with the type of medication and the amount that worked well for you in the hospital.
When you are at home, take your pain medication as you need it. You can also continue to hold ice chips inside your mouth to decrease pain and swelling. Use the pain medication in the same way as it worked in the hospital. Some days may be worse than others, and it may be frustrating because the pain continues at roughly the same level for 10-14 days after surgery. Try not to let the pain increase until it becomes intolerable before you take the medication. If you are running out of medication and need more, please call the office in advance to obtain another prescription. If you prefer to avoid narcotics, you should feel free to use acetaminophen (Tylenol®). Avoid aspirin, NSAIDs (such as ibuprofen, Advil®, Motrin®, naproxen, or Aleve®), vitamin supplements, or herbal medications for at least two weeks because they can increase your risk of bleeding after surgery. Your pain can be significant for at least the first 7-10 days following surgery, but it should improve markedly by 14 days following surgery.
Ice in the mouth
Holding ice in the mouth while they melt and cool the surgical area can help with pain control. Doing this for the first 3 days after surgery is somewhat similar to applying ice to a sprained ankle. It is one of the safest ways to reduce pain and can make the healing process easier.
Nutrition and fluids
It is very important to have good nutrition and avoid dehydration after surgery. Due to the pain and swelling that is expected after surgery, you will most likely only be able to tolerate a liquid diet for the first 4-5 days after surgery. Push yourself to drink fluids, even if it is painful. The first sign of dehydration is a decrease in urination, so keep track of this. In addition to water, it is It is helpful to drink other liquids, such as juices or Gatorade®. It is also essential that your body receive protein and fat in your diet to help with healing and maintaining your energy level. Every day, you should have 3 glasses of something with fat and protein like milk or chocolate milk, nutritional supplements like Muscle Milk® or Ensure®, or protein shakes. Dr. Kezirian may order a nutritional supplement like this while you are in the hospital. As your recovery continues, you will transition to soft solid foods such as eggs, yogurt, or mashed potatoes. You should be able to tolerate a fairly normal diet by 3 weeks after surgery. During the recovery period, you should avoid hard foods or foods with sharp edges such as chips because these can cause bleeding or otherwise interfere with healing of the roof of your mouth. Otherwise, you can advance your diet according to your own schedule, being careful not to cause too much pain. Dr. Kezirian wants his patients to maintain their nutrition so that they do not lose weight in the few weeks right after surgery.
Antibiotics
Most patients receive an antibiotic while in the hospital. You may be prescribed an antibiotic to take when you go home. This can be useful for preventing infection and decreasing swelling. Take the antibiotics as directed. When taking antibiotics, it can be helpful to eat yogurt that contains active cultures (usually a container will include these words) to minimize the risk of antibiotic-associated diarrhea. If you develop a rash or diarrhea (possible risks of antibiotics and other medications), stop the antibiotics and contact Dr. Kezirian immediately.
Activity
Walking after surgery is important. Patients should walk at least 3 times a day starting the day after surgery. Walking helps prevent blood clots from forming in your legs. Spending more time out of bed (walking or in a chair) than in bed is helpful because your lungs fill up with air, lowering the risk of fevers and pneumonia. Not walking enough is a major cause of fevers after surgery, so please do remember to walk at least 3 times every day. Patients should avoid strenuous activity for 4 weeks following surgery because that typically raises heart rate and blood pressure. For this reason, it can increase swelling or cause bleeding to start.
Do not use mouthwashes, lozenges, or throat sprays
Patients should not use mouthwashes, lozenges, or throat sprays following surgery because many of these contain alcohol or other chemicals that can irritate the lining of the mouth or numbing medication that can expose you to a serious complication when used for more than a couple of times.
Ear problems or jaw discomfort
The swelling in your throat that occurs after surgery can cause jaw pain or ear symptoms such as pain, pressure, or fullness. This is common and should improve within 1-2 weeks following surgery. It occurs because the soft palate and tonsils are next to the jaw and the small Eustachian tube that connects the space behind the eardrum to the top of the throat. Swelling in the throat can interfere with your ability to clear or pop your ears, and it can also be sensed by your body as pain coming from your ears even though the ears are not affected (a phenomenon called referred pain).
Sleep with head elevated (at 45 degrees) for at least three days
Elevating your head during sleep decreases blood flow to the head and neck regions. Therefore, it decreases swelling and the associated pain. Elevating the head during sleep may also improve breathing patterns in other ways. Therefore, we recommend elevating your head during sleep at 45 degrees for at least three days following the procedure.
Nausea and constipation
Nausea and constipation are very common after any surgery. The anesthetic medications that you receive during surgery and the narcotic pain medication you receive after surgery can cause these. You will receive medications after surgery to decrease nausea and constipation, but please notify Dr. Kezirian if you feel constipated or have not had a bowel movement in any 3 days after surgery.
Postoperative appointment
Dr. Kezirian likes to see his patients 1-2 weeks after surgery. If a postoperative appointment has not been scheduled, please contact the office to schedule this when you return home after your surgery.
Additional questions
For any emergencies, please call 911 or go to the nearest emergency room. For other questions, please call the UCLA Health System page operator at (424) 259-6700 and ask for the Head and Neck Surgery resident on call.



