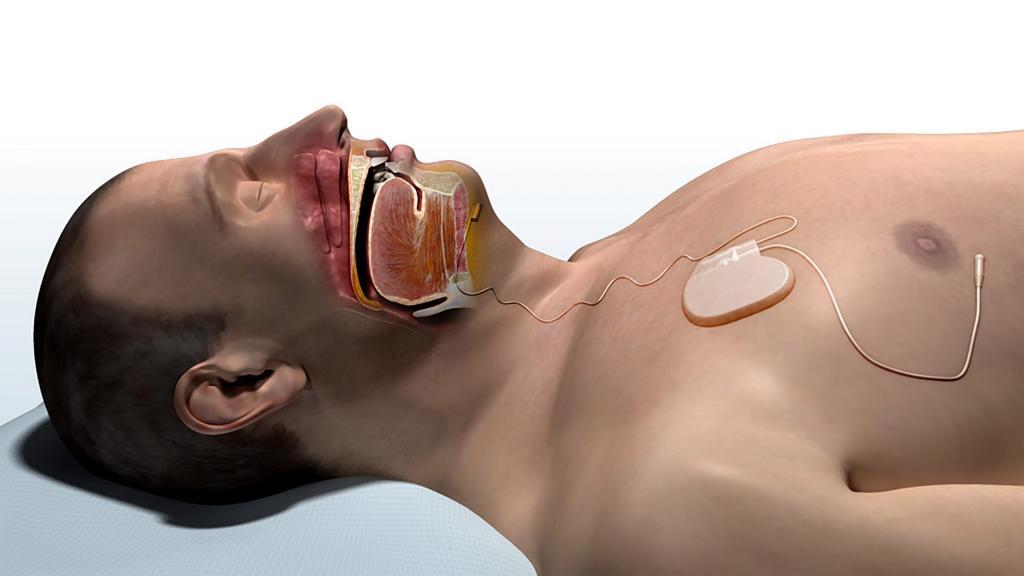
Inspire Upper Airway Stimulation for sleep apnea is a powerful and exciting treatment for many patients who do not succeed with positive airway pressure therapy (for example, CPAP or BPAP). Inspire Upper Airway Stimulation for sleep apnea is a system that involves a surgical procedure to implant 3 components. These components work together to deliver stimulation to the nerve that controls tongue movement (hypoglossal nerve) during sleep. I have been involved with hypoglossal nerve stimulation for the treatment of obstructive sleep apnea for over 7 years and have witnessed the major improvement in sleep apnea that can occur. We draw heavily on that experience in treating patients with sleep apnea, especially those who are treated with Inspire Upper Airway Stimulation for sleep apnea. I have written multiple times on this blog about Upper Airway Stimulation, including the following topics:
- how drug-induced sleep endoscopy is essential to selection of patients who will respond well to Inspire Upper Airway Stimulation
- results for Upper Airway Stimulation remain consistent, with a recent study following patients for 3 years
- because the benefits are substantial, the tradeoff between costs and benefits (called cost-effectiveness) is well within the range seen with many other medical devices
Inspire Upper Airway Stimulation for sleep apnea: not entirely just plug and play
Part of my speaking with patients before starting with Inspire Upper Airway Stimulation for sleep apnea is a discussion about how the system works. It is important for patients to understand that the surgery is the first step–but not the only step in the process. Once patients heal from surgery, the exciting part of treating their sleep apnea begins. There is what is called an activation visit where the device is turned on for the first time at a low level to allow a patient to get used to having the device on at night. This is a process called acclimation. Basically, it is a little odd at first for patients to have their tongue moving forward when they breathe in. There is no pain with the stimulation, but it is strange when it first happens. This is why the device is put on low settings, gradually building up the intensity of the stimulation (and tongue movement) over the course of about a month until the patient has a sleep study to determine the ideal system settings for them. Like CPAP, there is no single setting that is right for everyone.
Our interesting Inspire Upper Airway Stimulation case
An article that was just accepted for publication by the medical journal The Laryngoscope discussed our experience with one patient after the Inspire Upper Airway Stimulation system was turned on for the first time. Typically, there is a very low setting where a patient barely feels a twitch in their tongue (sensation threshold) and a higher setting where other people can see the tongue moving (functional threshold). In this one patient, these were the same, meaning that there was no setting to have the device barely moving the tongue before it moved more substantially.
As I mentioned above, substantial movement of the tongue is an odd feeling that can be disturbing for patients when they first experience it. What happened was that this patient contacted us with the sense that he was completely unable to sleep while wearing it and that the system must be malfunctioning. We obviously told him to turn off the device and come in to the office. We investigated this and saw that there were no problems with the system. In fact, the patient was then sent home at a setting lower than he felt when in the office, allowing him to adjust the settings as he became more comfortable with it on at night. I am happy to report that he is now sleeping better than he has in over 20 years, working out aggressively and lifting more weight at the gym than he has in a long time because he is finally getting some quality sleep!
The value of this experience
There were a number of important points that led us to share this experience with colleagues. First, with anything that does not seem right, patients should turn off the system and come in to the office for evaluation. Second, we always listen to patients but also explore a range of explanations for their experiences. This was not an electrical shock issue that might have been a system malfunction but was an unusual situation of having the sensation and functional thresholds be the same. Lastly, we rely on our experience and work with the outstanding team at Inspire Medical to come up with a solution that works. Once we develop a plan, we remain in close contact with patients to make sure that the problem is resolved.




24 + = 33