Previous blog posts have discussed our research centered on two large databases that include patients from centers around the world to examine how drug-induced sleep endoscopy findings are associated with outcomes of sleep apnea surgery. We have shown that specific different types of sleep apnea surgery and Inspire Upper Airway Stimulation. In this blog, I have also discussed how another study from our team using one of these databases added assessment of palate anatomy described by Tucker Woodson, MD to show that palate shape is associated with outcomes of Inspire Upper Airway Stimulation.
Emily Commesso, MD is now at Duke University after completing her sleep surgery fellowship training with me at USC. During her fellowship, she led similar work examining palate shape using the other multicenter database of patients undergoing surgery other than Inspire implantation. We had a fantastic team that included one of my sleep surgery colleagues at UCLA, Ashley Kita, MD. This research has just been accepted for publication and appeared online in the medical journal Otolaryngology – Head and Neck Surgery. In this study of 209 individuals undergoing sleep apnea surgery, palate was not broadly associated with surgery results when including all types of procedures. However, among the 76 study participants undergoing soft palate surgery alone, narrowing behind a bend in the muscle of the soft palate (called the GenuAP dimension, shown below) was associated with outcomes. Specifically, front-to-back narrowing was associated with poorer outcomes, while side-to-side narrowing was associated with better outcomes.
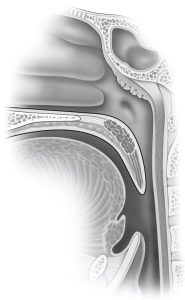
How could this be?
Soft palate procedures like the Australian modified palatopharyngoplasty or expansion sphincter pharyngoplasty are based on repositioning muscle and other soft tissue in an effort to move the soft palate forward and stabilize the sides of the throat. This study suggests that soft palate surgery may be limited in how much it can pull the soft palate forward when the bend of the soft palate muscle extends closer to the back of the throat. That being said, it supports the idea that these soft palate procedures do make a difference in collapse of the sides of the throat, an idea that has been proposed with only limited scientific evaluation.
How do I use this in caring for patients?
I was the first surgeon in the Western United States to offer Inspire therapy to patients after FDA approval in 2014 and remain a strong proponent of this approach. That being said, I believe that other surgical procedures still have an important role in treating obstructive sleep apnea. Last month, I wrote about a clinical trial that focuses on soft palate surgery, using medications to treat those who do not achieve resolution of their sleep apnea after surgery. This research is supported by the National Institutes of Health, one of the very few studies of its kind. We use drug-induced sleep endoscopy and have added palate shape – based on research studies like this one from our team – to identify patients who are the best candidates for soft palate surgery to include in the clinical trial. This is all based on our commitment to using the latest information to improve care of our patients and advance the science of sleep apnea surgery.




− 7 = 2